February is National Cancer Prevention Month, a time to focus on the impact of early cancer detection and prevention. As healthcare providers, you know that catching cancer in its earliest stages significantly improves patient outcomes. Advanced imaging technologies continue to play a crucial role in detecting cancers before they progress, giving patients the best chance for successful treatment. This is especially important for facilities in rural or underserved areas, where access to specialized medical services is more limited.
The Importance of Early Detection Through Imaging
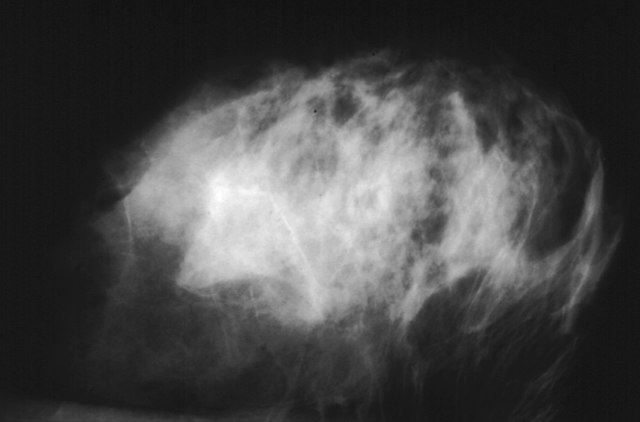
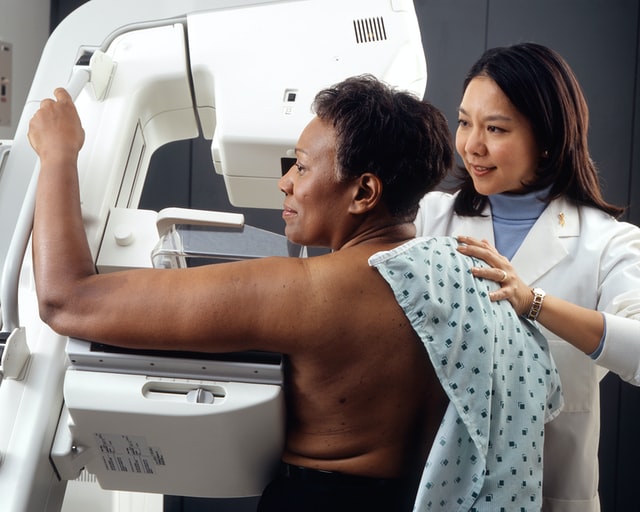
Early detection of cancer through imaging allows for interventions at stages when treatment is most effective. Techniques such as mammography, low-dose computed tomography (LDCT), and magnetic resonance imaging (MRI) are instrumental in identifying cancers like breast, lung, and prostate in their nascent stages. Regular screenings can lead to early diagnosis, which is associated with higher survival rates and a broader range of treatment options.
Teleradiology: Bridging the Gap in Underserved Areas
Teleradiology plays a pivotal role in expediting cancer diagnoses, particularly in rural or underserved regions. By transmitting radiological images from one location to another for interpretation by specialists, teleradiology ensures that patients receive timely and accurate diagnoses regardless of their geographical location. This technology mitigates the challenges posed by a shortage of on-site radiologists and enhances the quality of care in remote areas.
 Recent developments underscore the significant benefits of teleradiology for healthcare providers. A report from Healthcare IT News highlights how teleradiology enables radiologists to interpret scans remotely, increasing flexibility in work schedules and expanding access to specialized expertise. This approach addresses staffing challenges and enhances patient care by providing timely, expert interpretations.
Recent developments underscore the significant benefits of teleradiology for healthcare providers. A report from Healthcare IT News highlights how teleradiology enables radiologists to interpret scans remotely, increasing flexibility in work schedules and expanding access to specialized expertise. This approach addresses staffing challenges and enhances patient care by providing timely, expert interpretations.
Furthermore, a comprehensive guide by Philips emphasizes that teleradiology ensures 24/7 availability of radiology experts, allowing patients to receive timely diagnoses regardless of the time of day. This continuous access to radiological services helps alleviate the workload on in-house radiologists, leading to more efficient and focused patient care (Philips).
Additionally, RealTime Medical outlines several advantages of teleradiology, including cost savings, improved patient outcomes, increased efficiency, and better quality control. These benefits collectively enhance the overall performance of healthcare facilities by streamlining operations and ensuring high-quality diagnostic services.
Latest Screening Guidelines
Staying informed about current cancer screening guidelines is essential for both healthcare providers and patients. Here are the latest recommendations for breast, lung, and prostate cancer screenings:
- Breast Cancer: The American Cancer Society recommends that women aged 45 to 54 undergo annual mammograms. Women aged 40 to 44 should have the option to start annual screening if they wish, and those 55 and older can transition to biennial screening or continue yearly exams. Screening should continue as long as a woman is in good health and expected to live at least 10 more years (American Cancer Society).
- Lung Cancer: The U.S. Preventive Services Task Force advises annual screening for lung cancer with LDCT in adults aged 50 to 80 years who have a 20 pack-year smoking history and currently smoke or have quit within the past 15 years. Screening should be discontinued once a person has not smoked for 15 years or develops a health problem that substantially limits life expectancy (USPSTF).
- Prostate Cancer: The American Urological Association suggests that men aged 55 to 69 engage in shared decision-making with their healthcare provider about the benefits and risks of prostate-specific antigen (PSA)–based screening for prostate cancer. For men younger than 55 at higher risk, such as those with a family history of prostate cancer or African American men, discussions about screening may be appropriate (AUA).
Optimizing Radiology Practices
Healthcare facilities can enhance their radiology services by:
- Implementing Teleradiology: Adopting teleradiology services can provide access to subspecialty radiologists, reduce turnaround times for image interpretations, and offer continuous coverage, which is particularly beneficial for facilities in underserved areas.
- Investing in Advanced Imaging Technologies: Upgrading to the latest imaging equipment ensures higher resolution images, leading to more accurate diagnoses.
- Continuing Education for Radiologists: Encouraging radiology staff to engage in ongoing education keeps them abreast of the latest advancements and best practices in imaging and interpretation.
- Community Outreach and Education: Educating the community about the importance of regular screenings and early detection can lead to increased participation in screening programs, ultimately improving public health outcomes.
- Recent developments underscore the significant benefits of teleradiology for healthcare providers. A report from Healthcare IT News highlights how teleradiology enables radiologists to interpret scans remotely, increasing flexibility in work schedules and expanding access to specialized expertise. This approach addresses staffing challenges and enhances patient care by providing timely, expert interpretations.
- Furthermore, a comprehensive guide by Philips emphasizes that teleradiology ensures 24/7 availability of radiology experts, allowing patients to receive timely diagnoses regardless of the time of day. This continuous access to radiological services helps alleviate the workload on in-house radiologists, leading to more efficient and focused patient care.
 By focusing on early detection through advanced imaging and leveraging teleradiology, healthcare providers can significantly impact cancer outcomes, offering patients the best chance for successful treatment. National Cancer Prevention Month serves as a reminder of the strides we can make in cancer care through prevention and early detection.
By focusing on early detection through advanced imaging and leveraging teleradiology, healthcare providers can significantly impact cancer outcomes, offering patients the best chance for successful treatment. National Cancer Prevention Month serves as a reminder of the strides we can make in cancer care through prevention and early detection.
At Vesta Radiology, we are committed to leveraging the advantages of teleradiology to provide exceptional diagnostic services. Our team of experienced radiologists is available both on-site and remotely, ensuring that healthcare providers receive timely and accurate interpretations tailored to their specific needs. By partnering with us, facilities can enhance their radiology services, improve patient outcomes, and optimize operational efficiency.
For more information about our services and how we can support your healthcare facility, please visit our website at Vesta Radiology.