The U.S. healthcare system is in the midst of a critical radiologist shortage — and the numbers in 2025 make this shortage impossible to ignore. Demand for imaging services has surged post-pandemic, driven by an aging population, expanded access to preventive care, and rising chronic disease rates. However, the number of practicing radiologists is not keeping pace.
The effects are already being felt: longer wait times for results, increased radiologist burnout, and unequal access to diagnostic care — particularly in rural and underserved communities.
According to a detailed forecast by the Harvey L. Neiman Health Policy Institute, even under optimistic scenarios, demand for imaging will outpace radiologist supply through 2055. The study projects that while the radiologist workforce could grow by 25.7% by 2055, utilization of imaging will rise by 26.9% depending on modality. In short, we’re adding radiologists — but not fast enough to meet need.
What’s Driving the Shortage?
Multiple systemic pressures are converging to create a sustained staffing gap in radiology. These include:
- Aging Workforce: A large portion of today’s practicing radiologists are nearing retirement, with few new specialists entering the field quickly enough to replace them.
- Education Pipeline Lag: Radiology requires years of post-medical school training, and while interest in the field remains strong, residency and fellowship slots are limited.
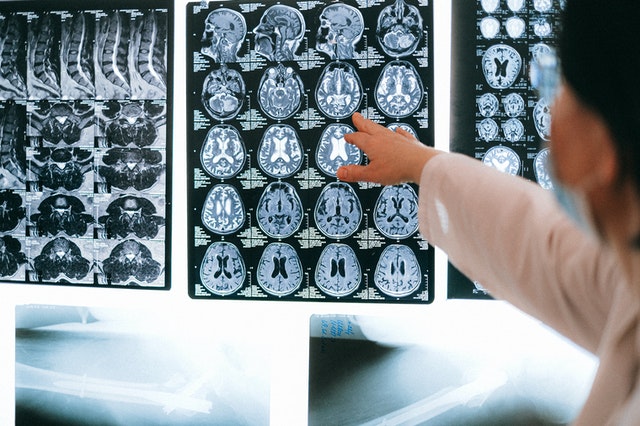
- Demand Surge: Advanced imaging like CT, MRI, and PET scans are being used more frequently — not only for diagnostics, but also to monitor treatment plans and disease progression.
- Rural Access Disparities: Smaller hospitals and imaging centers in less populated regions often can’t attract or retain radiology talent. That geographic imbalance further widens the care gap.
- Burnout and Exit Rates: Many radiologists are reporting unmanageable workloads. Increased case volumes and after-hours reading requirements have pushed some to reduce hours or exit clinical practice altogether.
Why It Matters: The Risks of Delayed Imaging
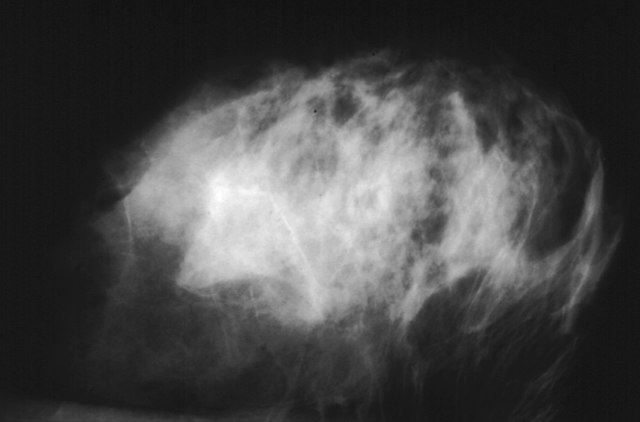
Radiology is a cornerstone of modern medicine. From early cancer detection to stroke response to monitoring for cardiac disease, delays in diagnostic imaging can significantly impact outcomes.
If a hospital or imaging center is understaffed, reports are delayed — and so are diagnoses and treatments. This delay is not just a logistical issue; it becomes a patient safety concern. Triage becomes more difficult. Non-urgent scans are de-prioritized. Referring providers may make decisions without complete imaging data, increasing risk.
The American College of Radiology has pointed to these challenges as serious enough to jeopardize care quality if not addressed through scalable solutions.
Teleradiology: A Modern, Scalable Response
Teleradiology — the practice of transmitting radiological images from one location to another for interpretation — has grown from a niche solution into a mainstream answer for today’s staffing shortages. Here’s why it works:
- Access to Subspecialists: Even small hospitals can now consult with neuroradiologists, musculoskeletal experts, or breast imaging specialists via remote platforms.
- 24/7 Coverage: Teleradiology groups provide overnight and weekend reads, reducing the burden on in-house teams and helping facilities maintain faster turnaround times.
- Rural Facility Support: Community hospitals that struggle to recruit full-time radiologists can partner with teleradiology providers for continuous coverage.
- Burnout Prevention: Teleradiology offers a flexible work model, which helps retain experienced radiologists who may not want a traditional on-site schedule.
Challenges and Considerations
While teleradiology offers clear benefits, it’s not without limitations. Facilities must ensure that:
- Images are transmitted securely and in compliance with HIPAA standards.
- Radiologists are appropriately credentialed at the site of care.
- Communication protocols are in place so that referring physicians can easily consult with off-site readers.
- Quality assurance is consistent, regardless of reader location.
When implemented correctly, however, these challenges are manageable — and the benefits are significant.
Looking Ahead: What Healthcare Systems Can Do
Healthcare systems can begin addressing this shortage in two ways: by growing the radiologist pipeline and by leveraging teleradiology and AI to scale services today.
Expanding residency positions, streamlining licensing across states, and adopting hybrid radiology staffing models are all part of the solution. But even with those improvements, the reality is that outsourcing some portion of reads to teleradiology providers will remain essential for years to come.
Conclusion
The radiologist shortage isn’t a temporary workforce hiccup — it’s a structural issue that will take decades to resolve. In the meantime, hospitals and imaging centers must adapt. Teleradiology is not a replacement for local staff — but it is a necessary extension of the radiology workforce. By tapping into its flexibility and reach, healthcare organizations can maintain diagnostic speed, quality, and equity — no matter where their patients are.