Why broader coverage matters in rural settings
Rural hospitals are asked to do a great deal with limited staff, tight budgets, and uneven access to specialty care. Imaging is part of that pressure every day. A smaller hospital may not need the same staffing model as a large urban system, but it still needs dependable support for a wide range of studies, including CT, MRI, mammography, nuclear medicine, and emergency overnight work.
A full-service radiology model helps close that gap. The issue is rarely just finding someone to read studies after hours. More often, hospital leaders are trying to build coverage that fits real volumes, supports multiple modalities, and gives clinicians timely answers when the case is urgent.
The challenge is continuity, not just coverage
That distinction is becoming more important. In an April 2026 discussion on rural radiology, the American Hospital Association highlighted the need for partnerships that help hospitals keep care local and avoid disruptions tied to staffing instability, retirements, and shifting group coverage. For rural facilities, continuity matters. The reading group has to feel like part of the care team, not a disconnected overnight vendor.
In practical terms, that means asking whether a radiology partner can support the hospital across the full imaging landscape. CT and MRI are central to that conversation because advanced imaging demand continues to grow. Vizient has pointed to continued expansion in CT and PET volume and sustained growth in outpatient and hospital-based imaging demand, which means small hospitals cannot afford to think only about today’s schedule.
A better fit for low-volume overnight needs
Many rural hospitals sit in an in-between category. They may not have the volume to justify round-the-clock in-house subspecialty staffing, yet they still treat stroke symptoms, trauma, abdominal pain, oncology patients, and other cases that require timely reads. Low-volume overnight coverage is where a flexible partner can make the biggest difference.
The right model supports overnight preliminary or final reads without forcing a hospital into an arrangement built for a much larger facility. It should also account for modality mix. A hospital that depends on CT after midnight has different needs than one that is mainly handling basic X-ray work.
Why modality depth and subspecialty access matter
Mammography and nuclear medicine deserve attention here as well. These are not side considerations for many community facilities. They often involve more scheduling coordination, tighter reporting expectations, and a stronger need for specialized interpretation. When hospitals rely on patchwork coverage, the first stress points often show up in the studies that require deeper expertise or more reliable workflow.
That is why radiology directors and hospital administrators should look beyond simple turnaround promises. The better questions are whether the group can read across modalities, whether subspecialty support is available when the case calls for it, and whether communication is strong enough to support real clinical decision-making.
Planning for a tighter workforce environment
The workforce backdrop makes this even more relevant. The American College of Radiology reported in 2026 that radiologist attrition rates more than doubled from 2014 to 2022, with higher attrition in practices serving rural sites. That does not mean rural hospitals are out of options. It does mean they benefit from partners built for stability, flexible coverage, and long-term relationships.
For hospitals under 100 beds, full-service radiology coverage is often less about having every radiologist on site and more about having the right structure in place. A combination of on-site and remote support, broader modality coverage, overnight availability, and dependable communication can help protect local access without overextending internal teams.
What hospital leaders should look for
The hospitals that navigate this well usually move beyond the question of who can cover nights. They look for a radiology partner that can support the service line as a whole. That includes advanced modalities, low-volume overnight reads, subspecialty access, and a workflow that fits the hospital’s day-to-day reality.
For rural hospitals trying to keep care close to home, that kind of partnership can make a meaningful difference.
FAQs
What does full-service radiology coverage mean for a rural hospital? It usually means support across multiple modalities and workflows, which may include on-site and remote coverage, overnight reads, subspecialty access, and interpretation beyond basic X-ray and ultrasound.
Why is low-volume overnight coverage important? Even hospitals with modest overnight volume still face urgent clinical decisions. Timely imaging interpretation can support emergency care, admissions, transfers, and treatment planning.
Which modalities should hospitals consider when evaluating a radiology partner? Many facilities should look beyond X-ray and ultrasound and ask about support for CT, MRI, mammography, and nuclear medicine based on their patient mix and service lines.
Why Rural Hospitals Partner With Vesta Teleradiology
For rural hospitals working to maintain access, improve turnaround times, and support a wider range of imaging needs, the right radiology partner can help create a more stable path forward. Vesta Teleradiology supports rural hospitals in key markets including Texas, California, Florida, Georgia, Illinois, Ohio, North Carolina, and Kentucky, providing full-service radiology coverage for CT, MRI, mammography, nuclear medicine, X-ray, ultrasound, and overnight reads. With flexible on-site and remote support, Vesta helps hospitals strengthen coverage without overextending internal teams.
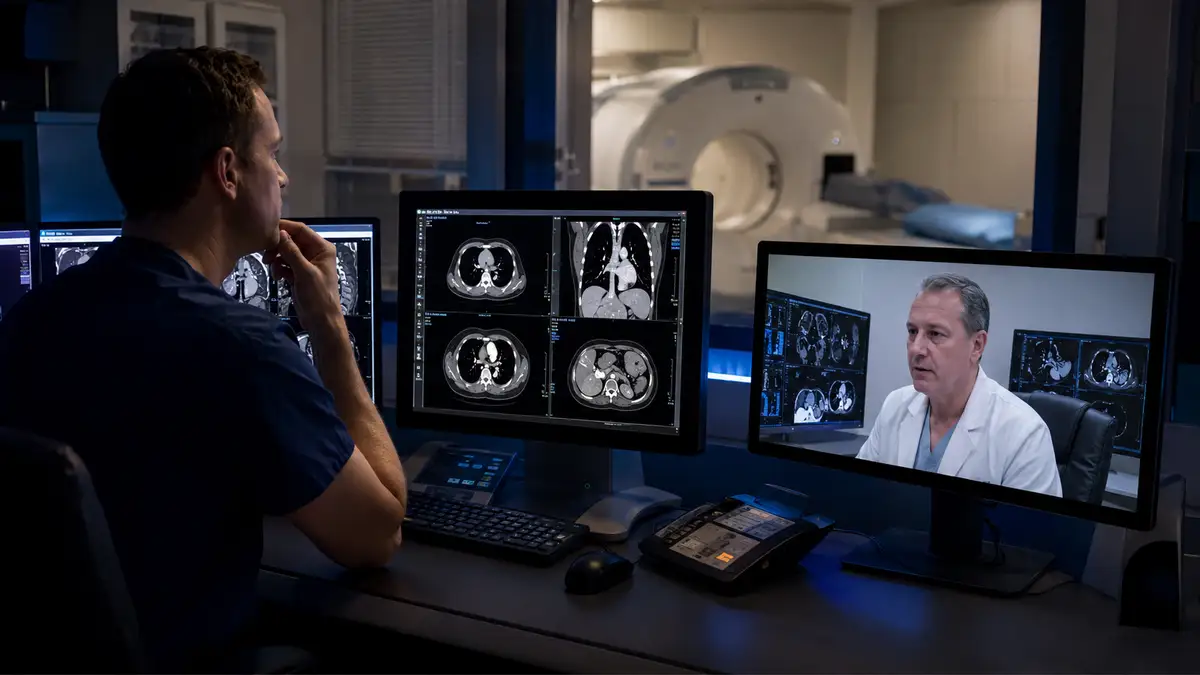





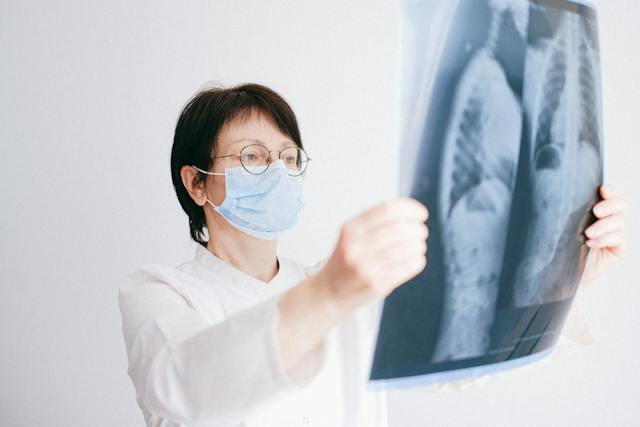


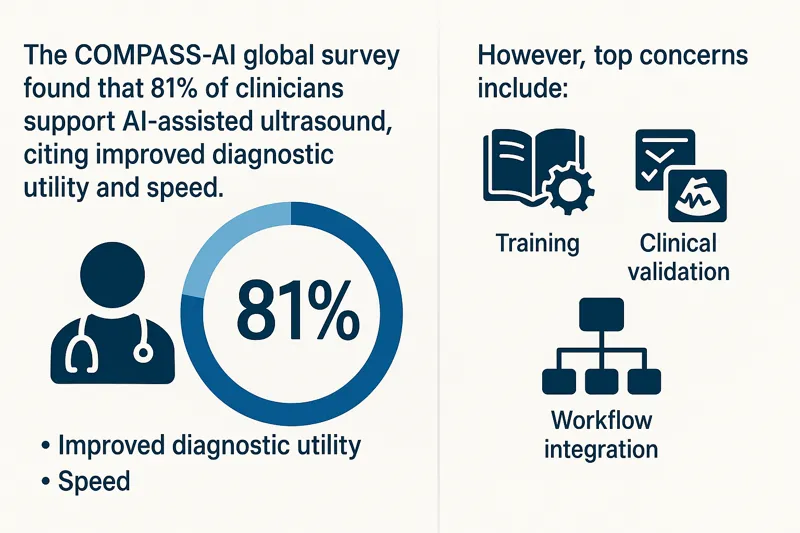
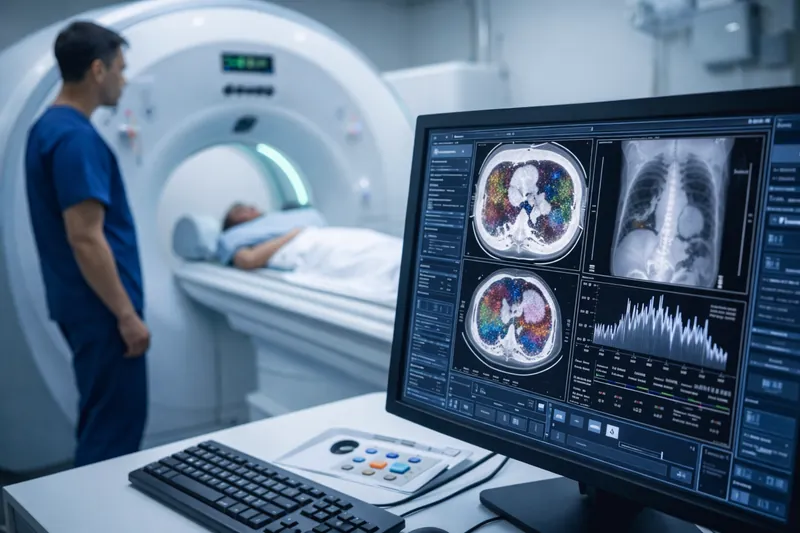 Across 2025 literature and trade coverage, the narrative tightened around what administrators care about: clearer visualization and characterization, potential dose efficiencies, and broader specialty applications as the evidence base grows.
Across 2025 literature and trade coverage, the narrative tightened around what administrators care about: clearer visualization and characterization, potential dose efficiencies, and broader specialty applications as the evidence base grows. Operational takeaway:
Operational takeaway:



 Why It Matters for Facilities and Radiology Teams
Why It Matters for Facilities and Radiology Teams