Why breast density remains a frontline issue
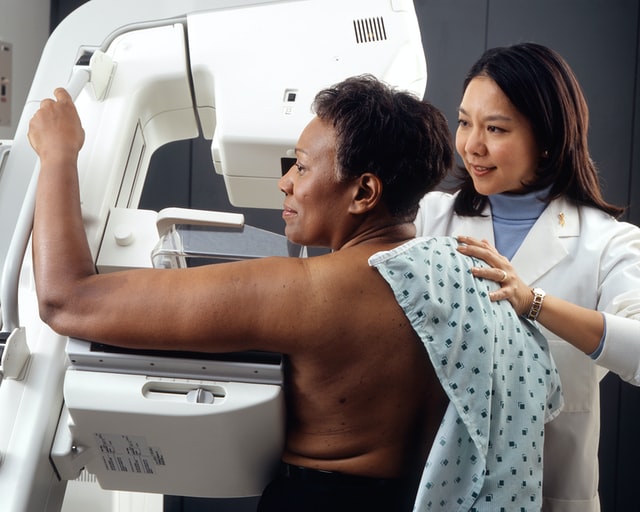
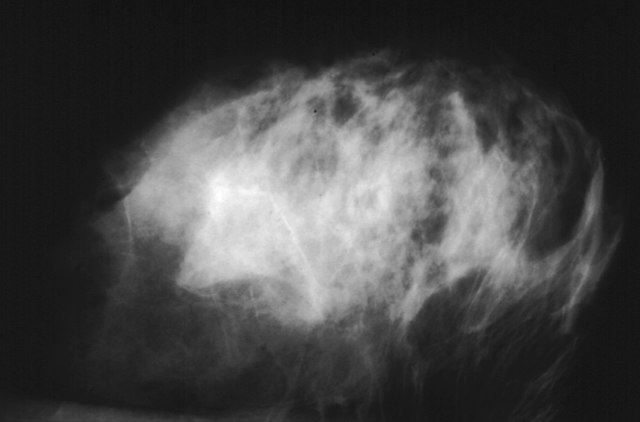
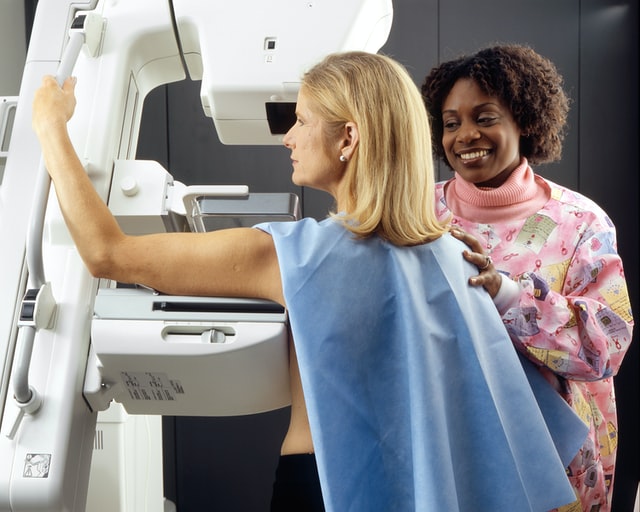
Breast density continues to be one of the most important—and complex—factors in breast cancer screening. Dense breast tissue not only raises cancer risk but also makes abnormalities harder to detect on mammograms. For hospitals and imaging centers, keeping up with evolving regulations, trial data, and technology is no longer optional. It’s central to compliance, patient communication, and imaging strategy.
FDA updates the national reporting standard
In July 2025, the FDA approved changes to the breast density reporting standard under the Mammography Quality Standards Act (MQSA). This builds on the September 2024 rule requiring that all mammography reports inform patients whether their breasts are “dense” or “not dense.”
Hospitals should review their reporting templates now. The updated language affects how results must be communicated to both patients and referring clinicians. Staying compliant avoids liability and ensures consistent, patient-friendly communication across facilities.
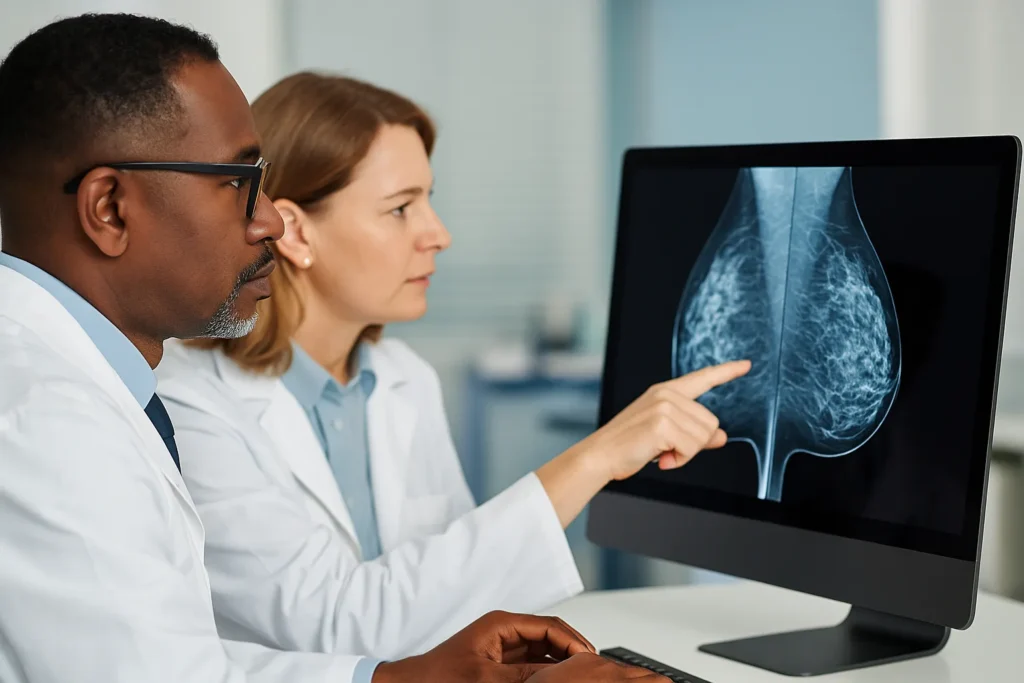 New trial evidence favors MRI and contrast-enhanced mammography
New trial evidence favors MRI and contrast-enhanced mammography
The interim results of the BRAID trial in the U.K. made headlines this summer. Among women with dense breasts and negative mammograms, supplemental abbreviated MRI and contrast-enhanced mammography (CEM) identified significantly more invasive cancers than ultrasound.
- MRI and CEM: ~15–19 extra cancers detected per 1,000 women screened
- Ultrasound: ~4 extra cancers detected per 1,000
These findings were reported in the OBG Project’s summary of the BRAID interim results.
While recalls and contrast risks remain a concern, the data strengthen the case for offering advanced supplemental imaging in high-density populations. Hospitals may want to begin planning how to integrate MRI or CEM into workflow, or establish referral pathways for patients with very dense breasts.
MBI joins the conversation
Molecular breast imaging (MBI), when paired with digital breast tomosynthesis, is showing early promise in improving invasive cancer detection in women with dense breasts. Findings from the Density MATTERS trial highlight MBI as a potential alternative for hospitals with limited MRI or CEM capacity.
AI-enabled density assessment and multimodal risk stratification
Artificial intelligence tools are advancing rapidly in breast imaging. A recent clinical study demonstrated that multimodal AI systems can reduce recall rates by over 30% while maintaining sensitivity. Other work shows promise in improving density quantification and developing 5-year breast cancer risk models from imaging features.
Hospitals considering AI adoption should focus on how these tools can streamline workflow, support compliance, and reduce unnecessary patient callbacks.
Shifting clinical culture: from notification to action
At the 2025 Society of Breast Imaging annual meeting, a clear theme emerged: simply notifying patients about dense breast status is not enough. The expectation is shifting toward offering supplemental imaging or providing clear, individualized next steps.
Hospitals that rely on tomosynthesis alone may increasingly be asked to justify why they do not offer MRI, CEM, or other supplemental options.
Key takeaways for hospitals and imaging centers
- Compliance check: Ensure your reporting language matches the updated FDA standard.
- Workflow planning: Prepare for increased demand for supplemental imaging in dense-breast populations.
- Technology assessment: Evaluate the role of MRI, CEM, MBI, and AI tools in your facility.
- Patient communication: Move beyond dense-breast notification toward structured shared decision-making.
- Equity focus: Consider insurance coverage and access barriers that could affect your patient population.
Hospitals that adapt now will not only stay compliant but also lead in patient-centered breast cancer screening strategies.