Every year on March 30, National Doctors’ Day recognizes the skill, commitment, and daily impact of physicians across the country. The American Medical Association describes it as an annual observance honoring physicians’ dedication to delivering high-quality care. In 2026, that recognition feels especially important as hospitals and health systems continue to manage physician shortages, growing imaging demand, and the pressure to maintain fast, high-quality care across every hour of the day.
When people think about physicians on the front lines, they often picture emergency medicine doctors, hospitalists, surgeons, and specialists seeing patients in person. But radiologists are physicians too, and behind the scenes, they play a major role in helping those care teams move patient care forward. Through teleradiology, that expertise can reach hospitals, imaging centers, and providers whenever it is needed most.
For many hospitals, especially those needing overnight, weekend, holiday, or subspecialty coverage, teleradiology is one of the support systems that helps physicians make timely decisions with greater confidence. Vesta Teleradiology positions itself as a Joint Commission-accredited, 24/7/365 provider serving hospitals, imaging centers, and health systems nationwide with U.S. board-certified radiologists and subspecialty support.
Helping Physicians Get Answers Faster
For emergency physicians and inpatient teams, waiting on an imaging interpretation can slow down patient flow, delay treatment decisions, and add pressure to an already demanding shift. That is one reason teleradiology matters so much behind the scenes. The right partner helps make sure studies are read promptly, critical findings are surfaced quickly, and referring physicians have the information they need when they need it.
This support is even more meaningful today because physician workforce strain is not easing. AAMC says the United States is projected to face a physician shortage of between 13,500 and 86,000 physicians by 2036, and ACR recently highlighted radiology workforce shortages and rising imaging volumes as a continuing challenge for the field.
Supporting Physicians Beyond After-Hours Coverage
Modern teleradiology is about more than reading cases at night. Hospitals increasingly need dependable coverage models that support physician teams around the clock, fill subspecialty gaps, and integrate smoothly into existing operations. That can mean helping a hospitalist get a faster final interpretation, supporting an ED physician with urgent reads overnight, or giving a facility access to subspecialty expertise that may not be available locally. RSNA has noted that radiology demand continues to outpace radiologist capacity, which adds to the importance of scalable support models.
Vesta’s service positioning reflects that broader support role. The company highlights 24/7 coverage, subspecialty interpretations, support for hospitals and imaging centers, and service across all 50 states.
Why This Matters for Rural and Underserved Communities
National Doctors’ Day is also a good time to recognize the physicians serving rural and underserved communities, where access challenges can be even more severe. Federal telehealth guidance continues to emphasize how telehealth can expand access in rural settings, and HRSA’s telehealth office exists specifically to improve access to quality care through integrated telehealth services.
For imaging, that can translate into meaningful operational support. Teleradiology can help hospitals maintain coverage when local recruiting is difficult, when internal teams need backup, or when subspecialty interpretation is not available onsite. Vesta also specifically connects its AI-assisted imaging strategy to benefits for both large health systems and rural or underserved communities.
The 2026 Angle: AI as a Support Tool, Not a Substitute
Another meaningful part of this discussion is the growing role of AI in helping physicians and radiologists manage workload. In 2026, hospital leaders are asking more practical questions about AI: Can it help prioritize worklists? Can it support faster review? Can it improve workflow without compromising physician oversight?
That is the right way to approach it. AI is most useful when it works in support of physicians rather than trying to replace clinical judgment
A Good Time to Recognize the Physicians Behind the Images
Doctors’ Day is not only about the physicians patients see face-to-face. It is also a reminder to appreciate the many physicians working behind the scenes to help every care decision happen. Radiologists, subspecialists, and the teleradiology teams supporting hospital operations are part of that story.
For hospitals in 2026, one of the most practical ways to support physicians is to strengthen the systems around them. Reliable teleradiology coverage, subspecialty access, and AI-enhanced workflow can help reduce bottlenecks, improve responsiveness, and make it easier for physicians to focus on patient care. On National Doctors’ Day, that is a worthwhile reminder: supporting doctors does not only mean celebrating them. It also means giving them the tools, coverage, and partnerships that help them do their jobs well.



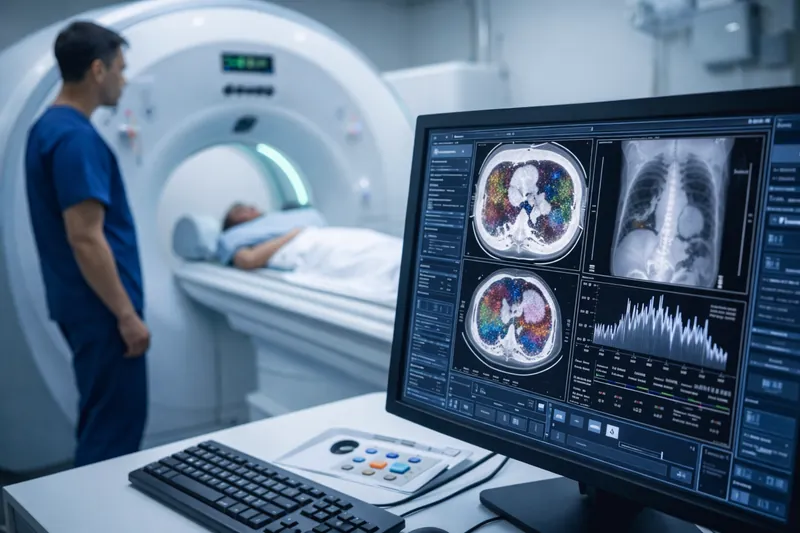 Across 2025 literature and trade coverage, the narrative tightened around what administrators care about: clearer visualization and characterization, potential dose efficiencies, and broader specialty applications as the evidence base grows.
Across 2025 literature and trade coverage, the narrative tightened around what administrators care about: clearer visualization and characterization, potential dose efficiencies, and broader specialty applications as the evidence base grows. Operational takeaway:
Operational takeaway:



 The Growing Demand for Subspecialty Reads
The Growing Demand for Subspecialty Reads

 However, challenges remain, including concerns about transparency in AI decision-making and biases in data sets. These hurdles are gradually being addressed with stricter regulations and improved algorithm training. AI isn’t just a tool; it’s becoming a trusted collaborator in radiology practices worldwide.
However, challenges remain, including concerns about transparency in AI decision-making and biases in data sets. These hurdles are gradually being addressed with stricter regulations and improved algorithm training. AI isn’t just a tool; it’s becoming a trusted collaborator in radiology practices worldwide. Radiology practices are adapting to these regulations by enhancing their reporting systems and educating patients about the implications of breast density. This legislation empowers patients to make informed decisions about supplemental screening options, improving early detection and outcomes.
Radiology practices are adapting to these regulations by enhancing their reporting systems and educating patients about the implications of breast density. This legislation empowers patients to make informed decisions about supplemental screening options, improving early detection and outcomes.