Radiology leaders have learned something uncomfortable: even if you have radiologist coverage, you can still have imaging gridlock. The reason is increasingly upstream—technologist staffing and capacity.
A widely cited ASRT survey highlighted a radiologic technologist vacancy rate of 18.1%, up from 6.2% only three years earlier, with real impact on patient scheduling and inpatient length of stay. Source: RSNA overview.
A separate summary for imaging executives echoed the same 18.1% vacancy figure and trend.
The practical takeaway: “radiology staffing” is no longer just a radiologist conversation. Here’s a leader-focused playbook to reduce delays without lowering standards.
How the tech shortage shows up in real metrics
You’ll usually see it in one (or all) of these:
- Longer time-to-scan (schedule access deteriorates)
- Higher no-show / reschedule rates (patients can’t find workable slots)
- More repeats (fatigue + rushing increases error risk)
- Backlogs that “mysteriously” worsen after holidays, flu surges, or PTO season
A 6-step action plan to reduce delays fast
1) Separate “demand” from “avoidable demand”
Not all imaging volume is equally necessary.
- Review repeats, protocol errors, and “wrong exam” orders.
- Tighten ordering pathways with clinicians (standardize indications and exam selection).
Even a small drop in repeat imaging can return capacity.
2) Standardize protocols to reduce tech time per exam
Protocol sprawl increases cognitive load and exam duration.
- Build a lean “default” protocol set for top 20 exams.
- Use tech-friendly checklists for complex exams (MRI safety, contrast workflows).
- Reduce variations across sites in a system.
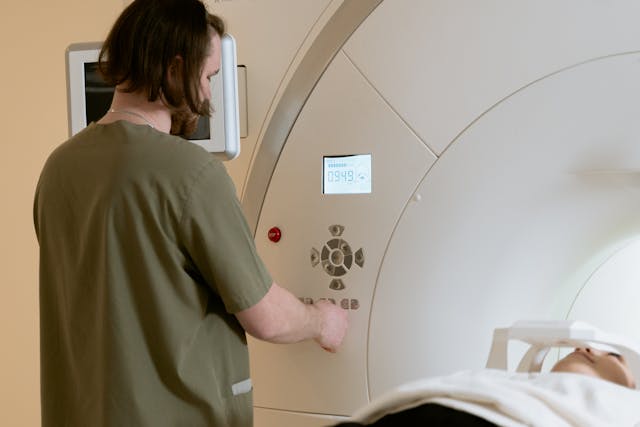 3) Smooth scheduling around your true capacity
3) Smooth scheduling around your true capacity
Stop scheduling to an ideal world.
- Build schedules around realistic staffing (including breaks, transport delays, and room turnover).
- Protect blocks for ED/inpatient add-ons so outpatient doesn’t implode daily.
- If you have multiple scanners, assign “quick win” exams to specific rooms to reduce reset time.
4) Use role design to protect your scarce talent
If your MRI tech is doing tasks that don’t require MRI training, you lose throughput.
- Shift non-licensed tasks away from techs where possible (transport coordination, documentation steps, room prep).
- Cross-train strategically (don’t cross-train everyone on everything—target the biggest bottlenecks).
5) Measure the right bottleneck metrics
Leaders often track report turnaround time but miss the upstream constraint.
Add:
- order-to-scan time
- scan-to-dictation start time
- exams per tech hour
- repeat rate (by modality and shift)
6) Backstop interpretation capacity so tech gains don’t get wasted
When tech workflows improve, volume rises—and the next bottleneck becomes reading capacity.
This is where flexible interpretation support helps protect throughput:
- prevent end-of-day reading pileups
- keep ED reads moving after-hours
- maintain consistency when staffing fluctuates
7) Make backlog reduction a burnout intervention
Overnight backlog doesn’t only harm metrics—it burns people out. A calmer, more predictable workflow improves clinician experience and decreases error risk.
Where Vesta fits
Vesta Teleradiology supports hospitals and imaging programs that want to keep overnight and weekend imaging moving—with dependable coverage and consistent interpretation quality. The goal is simple: fewer backlogs, steadier turnaround times, and smoother ED throughput.


 Why It Matters for Facilities and Radiology Teams
Why It Matters for Facilities and Radiology Teams
 Growing Market and Adoption
Growing Market and Adoption




 Sources:
Sources: